Educational video describing pressure measurement and fasciotomy.
my new book about compartment syndrome
[ Ссылка ]
A traumatic injury, such as a fracture of one of the long bones in the body (tibia), can often trigger acute compartment syndrome. The patient will complain of severe pain and narcotic requirements are usually increased. The trauma from injury or surgery will cause the limb to continue to swell. The cast is dressing will need to be removed so the limb can be inspected to rule out the presence of impending compartment syndrome.
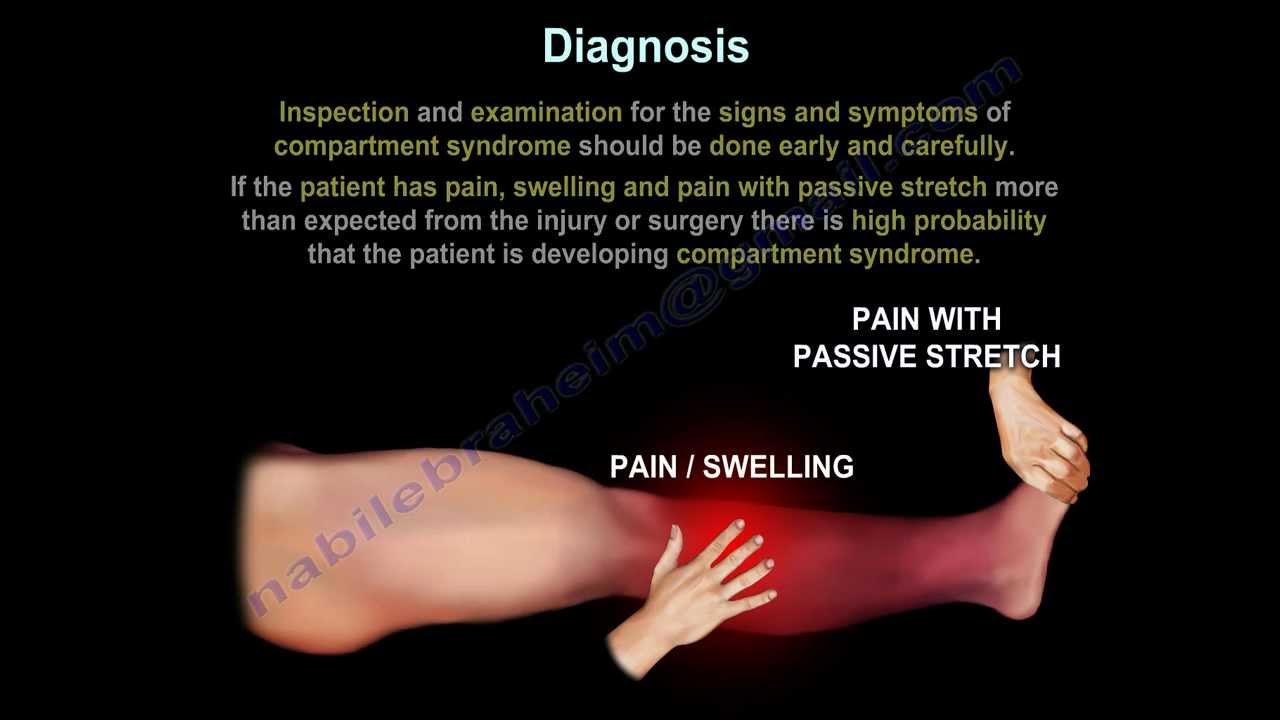
Inspection and examination for the signs and symptoms of compartment syndrome should be done early and carefully. If the patient has swelling, pain and pain with passive stretch more than expected from the injury or surgery there is high probability that the patient is developing compartment syndrome.
Do not wait for all 5 P’s to appear, as these findings are considered ate findings:
•Pain/swelling
•Pulselessness
•Paresthesia
•Pallor
•Paralysis
If compartment syndrome is suspected, compartment pressure should be measured. If the pressure exceeds 30 mmHg or within 30 mmHg form the diastolic pressure, immediate fasciotomy is necessary.
The intracompartmental pressure of 30 mmHg is the generally accepted value for diagnosis. Opposing values have been suggested.
Relative pressure (perfusion pressure gradient)
P = diastolic blood pressure- intracompartmental pressure.
Decompression of the involved compartments is indicated if the P falls to under 30 mmHg.
The value of the diastolic blood pressure in a patient under anesthesia with suspected compartment syndromes questionable. Do not rely on these values to get accurate information of the p. DBP under anesthesia is usually less.
Location of pressure monitor insertion is based on the etiology. A localize injury, especially a fracture, creates pressure gradient in the surrounding tissue that peaks within 5 cm of the injury. Intra-compartmental pressure should be taken within this range to avoid misdiagnosis. Vascular injury and repair lead to reperfusion edema in the entire area of ischemia. The pressure gradient around the injury is therefore more diffuse, so the location of the needle insertion does not have to be as exact for the fracture or trauma.
Diagnosis: measuring the pressure is the most reliable method to confirm clinical diagnosis of compartment syndrome.. it is the most important step in establishing the presence of an early or impending compartment syndrome. Once the diagnosis is made, urgent fasciotomy should be done.
Solid state transducer intracompartmental catheter:
1-Turn device on
2-Attach the diaphragm chamber and 18 gm side ported needle to syringe.
3-Place the needle-syringe assembly into the STIC motor unit
4-Close cover of the unit.
5-Slowly depress the plunger to remove any air from diaphragm and needle.
6-Hold unit in direction of insertion and press zero
7-Mark and prep area where STIC is to enter the compartment
8-Inject local anesthesia
9-Gently insert STIC needle
10-Inject 0.3 cc saline to equalize the interstitial pressure
11-Once pressure come to equilibrium, the pressure may be read from the monitor.
The most common compartment test for compartment syndrome of the leg is the anterior tibial compartment.
The anterolateral incision is placed halfway between the fibular shaft and the tibial crest.
The posteromedial incision is placed 2 cm posterior to the posterior margin of the tibia.
Become a friend on facebook:
[ Ссылка ]
Follow me on twitter:
[ Ссылка ]



























































![[REST API на Golang #9] Создание и получение списков](https://i.ytimg.com/vi/KpTZuZE5HS8/mqdefault.jpg)














